| What is the imaging study to follow my cystic organs over time ?
MRI
MRI is the exam to document the progress of liver
and kidney cysts. Certain specialized PKD centers can
calculate the blood flow to the kidneys to determine renal perfusion (kidney blood flow) with MRI. According to the PKD CRISP study increased kidney blood flow is the first sign
that a treatment is working. The MRI study
might be preferable to CT because it uses radio waves with no radiation exposure. Radiation
is cumulative over a lifetime. MRI is costly and requires that
the individual remain in an enclosed space for a short period of time. There is open MRI
but better images are produced through a closed MRI. For more on the CRISP study findings:
CRISP - Magnetic Resonance measurements of renal blood flow
CRISP - Renal structure in early PKD
CRISP - Cyst number but not the rate of cystic growth is associated with PKD1 or PKD2 full article
CRISP - Cyst number but not the rate of cystic growth is associated with PKD1 or PKD2 abstract
CRISP - Article by Dr. Grantham
CRISP - Imaging progression in PKD
CRISP - Volume progression in PKD as an indicator of clinical outcomes
CRISP - MRI provides early alert as to progression of PKD
CRISP - Volume progression in PKD
CT
SCAN
CT examination is also useful for following cystic organs though there is the added exposure to radiation with a CT.
What is an MRI?
MRI Magnetic resonance imaging is a way of obtaining very detailed images of the body without x-rays. Instead, it uses a powerful magnetic field, radio waves, a rapidly changing magnetic field, and a computer to demonstrate whether or not there is an injury or some disease process present. A patient is placed within the MR scanner—typically a large, tunnel or doughnut-shaped magnet that is open at both ends. The magnetic field aligns atomic particles called protons that are present in most of the body's tissues. Radio waves then cause these particles to produce signals that are picked up by a receiver within the scanner.
ANEURYSM
What
imaging studies look at blood vessels?
MRI MRA
Prior to my surgery, I had a brain MRA to check for the possibility of any aneurysms. PKD'rs have a 30% increased risk for developing an aneurysm. The symptoms include experiencing the worst headache ever. Researchers are now looking into a genetic link through families with an incidence of aneurysm.
Many individuals cannot tolerate the enclosed space of an MRI/MRA machine
and for this reason claustrophobic individuals prefer a CT scan. CT scans expose individuals to radiation,
as do x-rays. The effects of these are cumulative over a lifetime. Despite the tight MRI space, I really enjoy getting
an MRI. It is almost like a sensory deprivation tank where I totally relax
and take a few moments exclusively for me. I just put on the head phones,
listen to soothing music and away I go. I ask for a nice triangle
wedge pillow under my knees. All succeed in making me very relaxed.
An angiogram, like a venogram involves dye and a catheter, which is threaded
into the body. It gives the best images when the doctors want to find
out if there is something going on within a blood vessel. With me, the MRA
was performed first and it showed nothing. Then the venogram was done; this showed a small blockage of only 10% of my inferior vena cava. The
angiogram / venogram is more sensitive when a specific diagnosis is needed. Usually
they perform a CT scan or MRI first. Venogram and angiogram are not without
risk. One is exposed to the dye, to the invasiveness of a surgical catheter
(a very small incision is made), and to radiation.
Because an MRI uses radio waves, it has some risk to certain patients
- individuals with pacemakers and indwelling magnetized metal
are among those not candidates for an MRI or MRA. If individuals have difficulties
with enclosed spaces, sometimes it is helpful to take a pre-medication
before the study, often prescribed by the doctor. And there is the loud
"rat-tat-tat" noise generated by the MRI machine itself. Earphones
or earplugs help this. An MRI uses a computer program to light up certain
areas of tissue, in this case the vessels of the brain. The MRA is a similar study
done with the same machine. It highlights mainly the arteries, veins and
vessels. Sometimes the terms are used interchangeably. I usually ask to
speak to the radiologist and I explain to him that my doctor wants to
know i.e. if I have an aneurysm. He will then set the MRI machine to the correct
settings and view the pictures taken from the study with this in mind.
MRA
For purposes of finding a cerebral aneurysm, MRA has totally replaced
the need for a catheter threaded x-ray angiography. MR Angiography is a noninvasive
method to evaluate the patency of blood vessels without resorting to invasive
conventional x-ray angiography. The latter requires insertion of a catheter
into an artery (usually in the groin) and carries a certain amount of
risk (infection, vessel rupture, hematoma, occlusion, embolism, allergies
to iodine dye, etc.). If one has an allergy to shellfish, this is a reason to avoid the iodine dye.
An MRA scan provides more detail than a basic MRI scan. It can help detect
problems of the arteries and veins, such as a bulge in the wall of an
artery (aneurysm), blockage of a blood vessel (by pressure from multiple cysts, fatty deposits or a
blood clot), or a tear in the inner lining of a blood vessel (dissection).
MRA
with GADOLINIUM alert
The FDA is evaluating important safety information about gadolinium-containing contrast agents and a disease known as Nephrogenic Systemic Fibrosis or Nephrogenic Fibrosing Dermopathy (NSF/NFD) that occurs in patients with moderate to severe kidney failure. New reports have identified a possible link between NSF/NFD and exposure to gadolinium containing contrast agents used at high doses for a procedure called Magnetic Resonance Angiography (MRA). An MRA test uses magnetic resonance imaging to take pictures of blood vessels. During an MRA test, a drug known as a gadolinium-contrast agent is injected into a patient’s vein so blood vessels can be distinguished from other nearby tissues.
NEPHROGENIC FIBROSING DERMOPATHY NFD/NSF
NFD/NSF is a skin disease. It does not cause diminished kidney functioning. Nephrogenic means the origin is within the kidneys (moderately or severely diminished functioning). The process origin is within the kidneys however nephrogenic fibrosing dermopathy is not a cause for diminished kidney functioning. It is similar to a rheumatoid disease of the skin that becomes systemic.
NFD/NSF ARTICLES:
Gadolinium-containing Contrast FDA
Omniscan safety update
Nephrogenic systemic fibrosis among liver transplants
FDA Public Health Advisory update
Medpage Gadolinium alert
A renal biopsy
Nephrogenic research
Nephrogenic Fibrosing Dermopathy
Gadolinium deposition in nephrogenic fibrosing dermopathy
FDA Gadolinium contrast agent alert
CT
SCAN VIRTUAL COLONOSCOPY
Virtual Colonoscopy uses ultra fast spiral multi-slice CT to look at the colon; these are sent to the radiologist who looks at it and makes a diagnosis. In children this requires no prep, so the diagnosis of Chron's Disease is more readily seen. With CT, a three-dimensional picture of part of the body is put together from a number of images. In Europe and a few centers in the United States, some centers are using magnetic resonance imaging (MRI) for virtual colonoscopy. MRI uses radio waves to produce images of the inside of the body. A potential advantage of MR imaging is that it doesn't expose the patient to radiation, as CT does. The procedure was first performed in 1994.
Frail, elderly patients are more easily examined by Virtual Colonoscopy. For a website that reviews what is colonoscopy click here.
COLONOSCOPY
The prep for standard colonoscopy for PKD'rs is GoLYTLEY or polyethylene glycol (PEG). Avoid fleets phosphate soda with kidney disease. More about polyethylene glycol. Review the pros and cons of virtual colonscopy vs standard colonscopy. A recent research published in the Journal of the American Society of Nephrology showed purgatives containing sodium phosphate are an under-recognized cause of chronic kidney failure in the United States. Common bowel-cleansing drugs that include sodium phosphate are Visicol, a prescription oral tablet, and the non-prescription product Fleet Phospho-soda. Researchers cite several potential factors that may contribute to the development of kidney problems from sodium phosphate solutions, including inadequate hydration, a history of high blood pressure and the use of nonsteroidal anti-inflammatory drugs. Researchers from the Columbia College of Physicians and Surgeons in New York reviewed 7,349 kidney biopsies in their facility between January 2000 and December 2004 and found 31 patients who had kidney damage that was consistent with phosphate toxicity. Two-thirds of them had taken oral phosphate solutions prior to having colonoscopies.
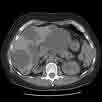
CT
SCAN
A CT exposes one to radiation. I had to lie on my spine for both
an MRI study and a CT study. To read more about CT scans click here.
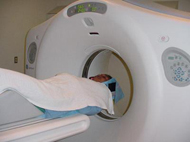
Are there risks
to obtaining a CT scan?
CT scan DYE
The most common problem is an adverse reaction to intravenous contrast
material. Intravenous contrast is usually an iodine-based liquid given
in the vein, which makes many organs and structures, such as the kidneys
and blood vessels much more visible on the CT scan. There may be resulting
itching, a rash, hives, or a feeling of warmth throughout the body. These
are usually self-limiting reactions and go away rather quickly. If needed,
antihistamines can be given to help relieve the symptoms. A more serious
reaction to intravenous contrast is called an anaphylactic reaction. When
this occurs, the patient may experience severe hives and/or extreme difficulty
in breathing. This reaction is quite rare, but is potentially life-threatening
if not treated. Medications which may include corticosteroids, antihistamines,
and epinephrine reverse this adverse reaction.
Toxicity to the kidneys which can result in kidney failure is an extremely
rare complication of the intravenous contrast used in CT scans. Diabetics,
dehydrated individuals, or patients who already have impaired kidney function
are most prone to this reaction. Newer intravenous contrast agents have
been developed, such as Isovue, which have nearly eliminated this complication.
Usually one must be fasting about 4 hours before having a CT scan done. If a woman were pregnant, then a better exam without radiation exposure
would be an ultrasound. Though radiation from a CT is minimal; during
the first three months of pregnancy, this exposure is too much for the
unborn fetus.
ULTRASOUND
or sonography, in medicine, technique that uses sound waves to study and
treat hard-to-view areas within the body. In scanning with ultrasound,
high-frequency sound waves are transmitted to the area of interest and
the returning echoes. First developed in World War II to locate submerged
objects, the technique is now widely used in virtually every branch of
medicine.
In obstetrics it is used to study the age, sex, and level of development
of the fetus and to determine the presence of birth defects or other potential
problems. Ultrasound is used in cardiology to detect heart damage and
in ophthalmology to detect retinal problems. It is also used to heat joints,
relieving arthritic joint pain, and for such procedures as lithotripsy,
in which shock waves break up kidney stones, eliminating the need for
surgery. Ultrasound is noninvasive, involves no radiation.
The radiologist is able to view an organ very close with great detail
within a water filled cyst vs. normal tissue. For an expansive view of
the organ in its entirety to determine size and the number of cysts, an
MRI or CT scan is needed.
An ultrasound is useful for determining if the blood vessels of the legs
are open and free flowing; also for determining the extent, which the
carotid arteries are blocked or open.
VENOGRAM
An venogram uses X rays to view your body’s blood vessels. This
is an invasive procedure usually reserved for those times when other imaging
studies are not sensitive enough to show a blockage, an aneurysm, or some
other vessel anatomy. Physicians use this test to determine the extent
of narrow, blocked, enlarged, or malformed arteries in many parts of your
body, including your brain, heart, abdomen, and legs. When the arteries
are studied, the test is called an arteriogram. If the veins are studied,
it is called a venogram.
An angiogram involves three major steps:
1)
insertion of a catheter (small tube) into your body
2)
taking x-ray pictures while contrast (x-ray dye) is being injected into
a vein,
3)
removal of the catheter.
CATHER INSERTION :
The staff will clean your skin with cold soap where the doctor will insert
the catheter. This is usually at the top of the leg (groin) or the upper
arm. You will then be covered with a sterile sheet. Next, the doctor will
use a small needle to numb your skin where the catheter will be inserted.
The nurse will give you medications in your IV to relieve the pain and
allow you to relax. You may feel pressure or brief discomfort as the catheter
goes in. The doctor will guide the catheter through the body to the vessel
that is to be studied by watching it on a TV-like monitor. You will not
feel the catheter moving through your blood vessels.
TAKING X-RAYS: Once the catheter
is in the correct vessel, contrast will be injected through the catheter
while x-ray pictures are being taken. You may feel hot inside when the
contrast is injected, but the sensation only lasts a few seconds. Several
series of contrast injections and x-ray pictures may be needed to complete
the examination.
REMOVAL OF THE CATHETER: When the angiogram
is completed, the doctor will remove the catheter from your blood vessel.
He/she will apply pressure for 10-15 minutes over the catheter site to
prevent bleeding. A band-aid will be placed on the insertion site. The
angiogram usually takes one or more hours to complete. The radiology staff
will always be nearby to keep you comfortable and answer any questions
you may have.
VENOGRAM
DYE
The dye is iodine based and may cause allergic reactions; it may affect
your kidney function causing a temporary rise in creatinine. For this
reason you are asked to drink plenty in order to flush the dye from your
bloodstream, to prevent dehydration and to help the contrast dye to exit
your body.
Fluoroscopy is often used during a renal venogram. Fluoroscopy is a study
of moving body structures - similar to an x-ray “movie.” A
continuous x-ray beam is passed through the body part being examined,
and is transmitted to a TV-like monitor so that the body part and its
motion can be seen in detail.
Risks to the vein in the groin
Quite often a small bruise ('hematoma') forms around the site where the
needle has been inserted. If this becomes a large bruise, then there is
a risk of it getting infected, and it may require treatment with antibiotics.
Very rarely, some damage can be caused to the artery by the catheter,
which may need to be treated by an operation or another radiological procedure.
Risks to the kidneys
The contrast material used to show up the arteries may temporarily worsen
kidney function. This is more likely if you have poor kidney function,
are a diabetic, or are taking some particular drugs.
Damage to other vessels
Moving tubes around in narrowed vessels can knock off tiny bits - 'emboli'
- which fly off and block much smaller veins in the feet, in the kidney,
or elsewhere. This is more likely if the vena cava (major blood vessel
from the heart) is badly narrowed, and occasionally it causes serious
trouble, for instance leading to kidney failure, or a need to amputate
toes or even limbs. Very rarely this can be fatal.
Risks from the dye
It is iodine based. If you are allergic to shellfish or have had a previous
reaction to iodine be sure to tell your doctor.
It is important to discuss what the risks are with the radiologist
and with the other doctors looking after you. The risks are very low for
most people, but higher for others.
I would like to get my liver cysts and kidney cyts evaluated
again. Which is the best test? Have you heard of a PET Scan?
PET scan
The PET
scan is useful to detect intrahepatic
cyst infections (inside the liver cyst infections); and especially for
detecting tumors or solid tumor masses. A PET scan uses glucose and replaces
one of the oxygen molecules with fluorine; a slightly radioactive substance
when attached to glucose goes right to solid tumor masses. This substance
is called 18Fluoro-2-deoxyglucose. University of Prague studied the use
of PET scan in panic disorders treated with antidepressants.
Changes in brain metabolism with (18)FDG uptake was similar in a number
of brain areas with prominent right-left differences. Another important
use for PET scan is for follow up studies after chemotherapy for Hodgkin’s
disease or lymphoma. The areas of tumor and lymph nodes light up with
increased uptake. According to a medical article, the standard PET
scan uptake is said to be an unreliable index with kidney disease.
Though PET scan has been used to diagnosis inside liver cysts infections,
the better study is a tagged white blood cell study. Blood is withdrawn
from the person. The cells are spun down and the white blood cells are
tagged and re injected back into the individual. The tagged white blood
cells go right to the infection like a magnet. The PET scan uses gamma
rays.
Ultrasound
For a first time test to rule out liver cysts or kidney cysts, the least
expensive test is an ultrasound. It is very good for determining if cysts
exist.
Gene Testing
If a family member is considering donating an organ and wants to be screened
for PKD, the better test would be an MRI. The definitive test would be
gene testing available through Athena Diagnostics with a cost with third
party insurance of $850. Additional family members could be tested for
$150 each.
CT scan
CT scan is a good procedure to determine the size of cystic organs and
the number of cysts. There are now available 16 head and 32 head CT scanner
imaging maChinese that produce gorgeous images. With a CT scan sometimes
iodine-based dyes are used. This can cause reactions and the CT scan
uses radiation to produce images. A CT scan is the procedure that is
used in most emergency rooms for middle of the night diagnosis. It is
useful for chronic ear infections, trauma, pulmonary embolus, stroke,
clots, liver cysts, kidney cysts and more.
MRI
MRI is the exam to document the progress of liver
and kidney cysts. With MRI certain specialized PKD centers can
calculate the blood flow to the kidneys to determine renal perfusion (kidney blood flow). According to the CRISP
radiographic study of PKD, reduced kidney blood flow is the first sign
that a treatment is not working well with PKD. The MRI study
might be preferable because it uses radio waves with no exposure to radiation. Radiation
exposure is cumulative over a lifetime. MRI is costly and requires that
the individual remain in an enclosed space for a short period of time. There is open MRI
but better images are produced with a closed MRI.
LIVER
CYSTS
Initially
I was told I had no liver cysts. My liver cysts were not discovered until
my bilateral nephrectomy 4 years after my kidney transplant.
I was 54. I had one liver cyst the size of a large orange
and about 6 the size of my thumb nail. Now, at age 57, I have a huge liver
cyst and all others are just as large.
The good news
is that at age 57 with 6-7 large liver cysts, you will probably not go on to develop
massive polycystic liver disease. I am not surprised that they did not see any liver cysts earlier. Imaging studies were not as developed prior to the development of CT scan and MRI. With these new imaging studies, fine imaging slices can be obtained that enable detection of very fine multiple liver cysts. The CRISP study also looked at the liver cysts. They found that 90% of individuals had liver cysts. If we all live to be old enough each of us will develop liver cysts. Liver cysts develop as we age. Most cause no problems.
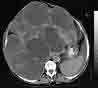 Probably we all have liver cysts if the imaging machine can make very thin cross sectional images. Probably we all have liver cysts if the imaging machine can make very thin cross sectional images.
Ultrasound was established as an imaging study as early
as 1978. It was quickly adapted for imaging of the fetus in utero because
its medium of transmission is sound waves that can see tissue surrounded
by water.
At that time this was the new procedure which could easily, non - invasively,
without the use of dyes, and with little risk to the patient, scan over
the tummy and show if an organ had fluid filled cysts. I did not have
my first ultrasound until I was 34 in 1981. My liver cysts were noted as too-many-to-count.
The nephrologist and the technician were both mumbling quietly and whispering
at my ultrasound images. I asked what was happening? The doctor explained
my liver was filled with cysts. They wanted a more detailed scan to be
sure that they were no masses and only fluid filled these numerous liver cysts.
IVP
Prior to that an IVP Intravenous pyelogram of my kidneys that showed one huge cyst on one
of my kidneys. This was done in 1960. No cysts were seen on my liver until the ultrasound was
performed in 1981. My liver was loaded with cysts.
The IVP examination is now used to diagnose painless hematuria provided
the doctor does not suspect that you might have a stone. If a person has
painful hematuria then they might do a CT.]
My oldest sister, who was 40 years my senior, had lost a lot of weight very
rapidly and the doctors could feel a mass within her belly. I was eight
years old. It was 1955. No imaging studies were available at this time.
The surgeons decided to operate as they thought she might have a cancer.
There was no hint that she had PKD and massive PLD.
Once they looked inside, she had severe polycystic liver disease and severe
polycystic kidney disease. Perhaps a cyst had become infected? She died
one week later of kidney failure.
The latest advances in imaging and medical treatments have made it possible
for me and others to diagnose massive liver cysts early.
I avoided exposure to hormones and thought of other alternatives to pregnancy.
It was not until 1985, that I avoided all caffeine when told by my nephrologist
to do so.
Through the deaths of my many family members, I have seen what things
seem to affect us with our particular set of genes and phenotype. This
knowledge has allowed me to continue to live a lifestyle that I thoroughly
enjoy.
I honor those who came before me so I could come to know some of the possible
courses of this disease. Today I am very healthy with stabilized liver
cysts and healthy kidneys and no hypertension. I also love and cherish
the unborn children that could have been, so that I am here today.
I talked with my husband last night and said I wish we could have had
a child. This was triggered by the fact that he is a new grandfather to
a bouncing baby girl weighing 5 pounds 13 ounces. He said to me very lovingly
and gently, ah, but then I would not have you here beside as we continue
to enjoy our aging together.
Ultrasounds
are done to detect cysts. How effective and accurate is this method?
What is the most accurate method of detecting any kind of cyst in the
organs, kidney and liver. I know there are MRI's and the other imaging procedures. What is a "cross section" of an organ?
MRI
MRI is best for detecting even small cysts. Ultrasound is good for an
immediate look at what is going on. It gives a close up view of what is
within the cyst - fluid, blood or infection.
Both use sound waves, radio waves and not radiation. CT scan uses radiation
as does x-rays.
The way MRI and CT scan works, is they photograph slices, cross sectional
slices through the abdomen. The size of these cross sectional slices can
be set to a millimeter or to a fraction of an inch. Cross section means
to slice an apple down the middle through the
core exposing apple seeds and apple flesh; this is a cross section. Then with
one of these halves, one could take several thin slices of through
the entire apple half so you would have a thin (cross sectional) slices. If it was thinner
than an apple seed, then you could get a half an apple seed in one cross
section, and the other half in the another cross section. As the (cross sectional) slices become thinner and thinner, the ability to detect small formed apple seeds becomes easier. It is the same with detecting
microscopic cysts.
Genetic
testing
There are false negatives from MRI.
If a family member is considering donating an organ, usually genetic testing is recommended in the absence of any cysts from an MRI. After age 30, there is a 5% chance
of false negatives with PKD1. After age 30 there is a 30% chance of false
negatives with PKD2. PKD1 gene is the more aggressive gene.
Breast MRI
Some of us in addition to having liver cysts have a family history of breast cancers. In women at high risk for breast cancer, here is an article recommending that we have both a breast MRI and a yearly mammogram.
last
updated
3-apr-08 3:06 PM
|
